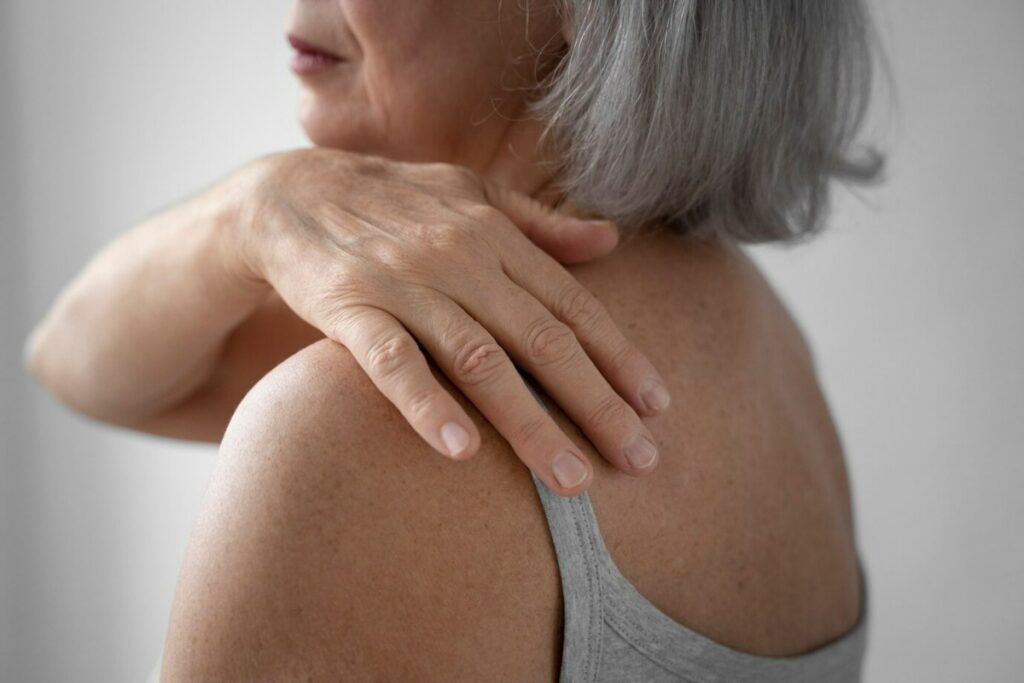
If you’ve ever experienced a gradual stiffening of your shoulder that makes it painful to lift your arm or reach behind your back, you may be dealing with a condition called frozen shoulder. This frustrating condition can significantly impact your daily activities, from getting dressed to reaching for items on a shelf. Here in Charlotte, NC, many patients visit Chiropractic Fitness wondering why their shoulder has become so stiff and painful, often without any obvious injury. Understanding frozen shoulder—what causes it, how to recognize it, and what conservative care options are available—can help you take the right steps toward recovery and regain the mobility you’ve lost.
What is Frozen Shoulder? Frozen shoulder, medically known as adhesive capsulitis, is a condition characterized by stiffness, pain, and progressive loss of range of motion in the shoulder joint. The shoulder capsule—the connective tissue surrounding the joint—thickens and tightens, restricting movement and causing discomfort that typically worsens over time before gradually improving.
Table of Contents
- Understanding Frozen Shoulder and How It Develops
- Common Causes and Risk Factors
- Recognizing the Symptoms and Stages
- How Frozen Shoulder is Diagnosed
- How Chiropractic Care Can Help
- Effective Management Strategies
- Prevention and Self-Care Tips
- When to Seek Professional Care
- Myths vs. Facts About Frozen Shoulder
- Final Thoughts
Understanding Frozen Shoulder and How It Develops
Your shoulder is one of the most mobile joints in your entire body, capable of moving in multiple directions to help you perform countless daily tasks. The shoulder joint is surrounded by a capsule of connective tissue that holds everything together while allowing fluid movement. In frozen shoulder, this capsule becomes inflamed, thickened, and tight, forming adhesions or bands of stiff tissue that restrict motion.
Unlike many shoulder injuries that result from trauma or overuse, frozen shoulder often develops without a clear precipitating event. The condition typically affects people between the ages of 40 and 60 and is more common in women than men. Research suggests that frozen shoulder affects approximately 2-5% of the general population, though certain groups face significantly higher risk.
The mechanics of frozen shoulder involve a complex inflammatory process. The synovial membrane that lubricates the joint becomes inflamed, and the capsule contracts and adheres to the head of the humerus bone. This creates a vicious cycle where limited movement leads to more stiffness, which further reduces your willingness or ability to move the shoulder, perpetuating the problem.
Common Causes and Risk Factors
While the exact cause of frozen shoulder isn’t always clear, several factors can increase your likelihood of developing this condition. Understanding these risk factors can help you recognize your vulnerability and take preventive steps when possible.
Prolonged Immobilization: One of the most common triggers for frozen shoulder is keeping the shoulder immobile for an extended period. This might occur after surgery, an injury, a fracture, or during recovery from a rotator cuff problem. When the shoulder doesn’t move regularly through its full range of motion, the capsule can begin to tighten and develop adhesions.
Metabolic Conditions: People with certain metabolic disorders face a substantially higher risk of frozen shoulder. Diabetes is particularly significant—individuals with diabetes have a 10-20% chance of developing frozen shoulder compared to 2-5% in the general population. The connection may relate to how elevated blood sugar affects collagen in connective tissues, making them more prone to stiffening.
Thyroid Disorders: Both hyperthyroidism and hypothyroidism have been associated with increased frozen shoulder risk. Thyroid hormones play important roles in tissue metabolism and repair, and imbalances may contribute to capsular changes in the shoulder.
Cardiovascular Disease: Research indicates that people with heart disease or who have experienced a stroke may be more susceptible to frozen shoulder. The mechanisms aren’t fully understood but may relate to systemic inflammation or reduced mobility during recovery periods.
Autoimmune Conditions: Conditions that involve immune system dysfunction or chronic inflammation appear to increase frozen shoulder risk. This includes conditions like rheumatoid arthritis, lupus, and other autoimmune disorders that affect connective tissues throughout the body.
Age and Gender: The condition most commonly affects people in their 40s, 50s, and 60s. Women experience frozen shoulder more frequently than men, though researchers haven’t definitively determined why this gender difference exists. Hormonal factors may play a role.
Previous Shoulder Injury or Surgery: Any trauma to the shoulder or surgical procedure in the area can trigger the inflammatory cascade that leads to frozen shoulder, particularly if post-operative rehabilitation doesn’t maintain full range of motion during healing.
Recognizing the Symptoms and Stages
Frozen shoulder is distinctive because it progresses through three well-defined stages, each with characteristic symptoms and duration. Recognizing which stage you’re in can help set realistic expectations for recovery and guide appropriate management strategies.
Stage 1: Freezing Stage (2-9 months): This initial stage is often the most painful. You’ll notice a gradual onset of shoulder pain that worsens over time, particularly at night. The pain may disrupt your sleep, especially when lying on the affected shoulder. During this stage, you begin to lose range of motion, and everyday activities like reaching overhead or behind your back become increasingly difficult. The pain is often described as a deep ache that can radiate down the arm. Many patients at Chiropractic Fitness in Charlotte describe this stage as the most frustrating because the pain seems to appear without warning or obvious cause.
Stage 2: Frozen Stage (4-12 months): During this stage, pain may actually decrease somewhat, but stiffness reaches its peak. Your shoulder becomes markedly restricted in all directions of movement—you may struggle to lift your arm away from your side, rotate it outward, or reach across your body. Simple tasks like putting on a jacket, fastening a bra, or washing your hair become challenging. The good news is that while stiffness is severe, the intense pain of the freezing stage typically improves. This stage represents a turning point where conservative care focused on maintaining and gradually improving mobility becomes especially important.
Stage 3: Thawing Stage (6 months to 2 years): This recovery stage brings gradual improvement in shoulder mobility. Range of motion slowly returns, though the process can be frustratingly slow. Some people recover completely, while others may experience some persistent limitation in motion. The thawing stage responds well to appropriate movement and therapeutic interventions aimed at restoring normal shoulder mechanics.
Common symptoms across all stages include difficulty with overhead activities, trouble reaching behind your back, disturbed sleep due to pain, and a feeling of tightness or tension deep in the shoulder joint. You might also notice compensatory changes in how you move—using your trunk or other arm more to accomplish tasks your affected shoulder can’t perform.
How Frozen Shoulder is Diagnosed
Diagnosing frozen shoulder involves a thorough clinical evaluation. At Chiropractic Fitness, Dr. [Doctor Name] begins with a detailed discussion of your symptoms, their onset, and how they’ve progressed over time. Understanding your medical history, including any history of diabetes, thyroid issues, or recent shoulder injuries, provides important context.
The physical examination is particularly revealing with frozen shoulder. Your chiropractor will assess both active range of motion—how far you can move your shoulder on your own—and passive range of motion—how far the shoulder can be moved when someone else guides it. In frozen shoulder, both active and passive motion are significantly restricted, which distinguishes it from conditions like rotator cuff tears where passive motion may be relatively normal.
Specific movement patterns help confirm the diagnosis. External rotation—rotating your arm away from your body with the elbow at your side—is typically the most restricted motion. Abduction—lifting your arm out to the side—is also significantly limited. These restrictions follow a characteristic “capsular pattern” that experienced practitioners recognize.
While imaging isn’t always necessary to diagnose frozen shoulder, X-rays or MRI may be ordered to rule out other conditions like arthritis, calcific tendinitis, or rotator cuff problems that can cause similar symptoms. These tests help ensure you receive the most appropriate care for your specific condition.
How Chiropractic Care Can Help
Chiropractic care offers a conservative, non-surgical approach to managing frozen shoulder that focuses on restoring proper joint mechanics, reducing inflammation, and gradually improving mobility. The goal isn’t to force the shoulder through painful movements but rather to work with your body’s natural healing processes while preventing further loss of function.
At Chiropractic Fitness in Charlotte, treatment for frozen shoulder is individualized based on which stage you’re experiencing. During the painful freezing stage, care emphasizes pain management and maintaining as much mobility as possible. This might include gentle mobilization techniques that move the shoulder within comfortable ranges, soft tissue work to address muscle tension and guarding, and modalities to reduce inflammation and discomfort.
As you progress into the frozen and thawing stages, care shifts toward progressively restoring range of motion. Chiropractors use specific joint mobilization techniques that apply controlled pressure to the shoulder capsule, helping to break up adhesions and stretch tight tissues. These techniques are performed gradually and systematically, respecting your pain tolerance while encouraging improvement.
Spinal adjustments may also play a role in frozen shoulder care. The shoulder and spine work together as an integrated system, and restrictions in the thoracic spine or ribs can contribute to shoulder dysfunction. Addressing these areas can improve overall shoulder mechanics and support better recovery.
Evidence from systematic reviews suggests that manual therapy and therapeutic exercise, cornerstones of chiropractic care, can be effective components of frozen shoulder management. The key is consistent, progressive treatment that adapts to your changing needs throughout the recovery process.
Your chiropractor will also provide guidance on therapeutic exercises you can perform at home. These exercises are crucial for maintaining and building on improvements made during office visits. They’re designed to be performed within comfortable ranges, gradually progressing as your shoulder permits.
Effective Management Strategies
Successfully managing frozen shoulder requires a comprehensive approach that extends beyond office visits. Here are evidence-based strategies that can support your recovery process.
Pendulum Exercises: These gentle exercises use gravity to create subtle motion in the shoulder without activating shoulder muscles that might be guarding. Lean forward with your good arm supported on a table, let your affected arm hang down, and create small circular motions or gentle swinging movements. Perform these several times daily to maintain mobility without aggravating inflammation.
Heat Application: Applying moist heat before stretching or movement can help relax tight tissues and improve flexibility. A warm shower or heating pad for 15-20 minutes can prepare your shoulder for gentle exercise. Heat is generally most helpful during the frozen and thawing stages when stiffness predominates over inflammation.
Ice for Pain Management: During the painful freezing stage, ice application after activity or at the end of the day can help manage inflammation and discomfort. Apply ice for 15 minutes at a time, using a barrier like a thin towel between the ice pack and your skin.
Maintain Movement: While it’s natural to protect a painful shoulder, complete immobility will worsen stiffness. Find ways to keep your shoulder moving gently within comfortable ranges throughout the day. Simple activities like using your arm during daily tasks, even if range is limited, helps prevent further capsular tightening.
Sleep Positioning: Pain often worsens at night with frozen shoulder. Try sleeping with your affected arm supported on pillows, either across your body or by your side. Avoid sleeping directly on the affected shoulder. Some people find sleeping in a recliner more comfortable during the most painful stage.
Stress Management: Chronic pain and limited function can create significant stress, which in turn can increase muscle tension and pain perception. Mind-body practices like deep breathing, meditation, or gentle yoga can help manage the psychological aspects of dealing with a lengthy recovery process.
Nutrition and Hydration: While no specific diet cures frozen shoulder, anti-inflammatory eating patterns may support overall healing. Focus on whole foods, adequate protein for tissue repair, and proper hydration. For patients with diabetes, maintaining stable blood sugar levels is particularly important.
Graduated Stretching Program: As your shoulder begins to thaw, progressive stretching becomes increasingly important. Your chiropractor at Chiropractic Fitness will design a specific program for you, but general principles include stretching to the point of mild tension without sharp pain, holding stretches for 20-30 seconds, and performing them consistently multiple times per day.
Prevention and Self-Care Tips
While not all cases of frozen shoulder can be prevented, certain strategies can reduce your risk, particularly if you have known risk factors or are recovering from a shoulder injury or surgery.
Maintain Regular Shoulder Motion: If you’re recovering from an injury or surgery, work closely with your healthcare providers to maintain shoulder mobility even during healing. Regular, gentle movement through available ranges helps prevent capsular tightening. Don’t let your shoulder remain completely immobile for extended periods unless specifically directed by your physician.
Manage Underlying Conditions: If you have diabetes, thyroid disease, or other metabolic conditions, work with your medical team to keep these well-controlled. Better management of these underlying conditions may reduce your risk of developing frozen shoulder.
Address Shoulder Problems Early: If you develop shoulder pain or notice decreased motion, seek evaluation sooner rather than later. Early intervention for shoulder problems may prevent progression to frozen shoulder in some cases.
Practice Good Posture: Rounded shoulders and forward head posture common in our modern, desk-based lives can contribute to shoulder dysfunction over time. Be mindful of your posture throughout the day. Take breaks from sitting, stretch your chest muscles, and strengthen the muscles between your shoulder blades.
Stay Active: Regular physical activity that includes shoulder movement in all directions helps maintain healthy capsular flexibility. Activities like swimming, yoga, or general exercise that incorporates arm movements can be protective.
Ergonomic Awareness: Set up your workspace to avoid prolonged positions that stress your shoulders. Your keyboard and mouse should be positioned so your shoulders remain relaxed, and your computer screen should be at eye level to prevent forward head posture that affects shoulder mechanics.
When to Seek Professional Care
If you’re experiencing shoulder pain and stiffness, especially if it’s worsening over time or significantly limiting your daily activities, it’s appropriate to seek evaluation from a chiropractor or other healthcare provider. Early assessment can help distinguish frozen shoulder from other conditions and get you started on appropriate management strategies.
Specific indicators that you should schedule an appointment at Chiropractic Fitness in Charlotte include shoulder pain that persists for more than a few weeks, progressive loss of motion that makes daily tasks difficult, pain that disrupts your sleep regularly, or shoulder symptoms accompanied by other concerning signs like numbness, weakness, or color changes in your arm or hand.
While frozen shoulder is typically managed conservatively, certain red flags warrant immediate medical attention. Seek urgent care if you experience sudden, severe shoulder pain following an injury, complete inability to move your shoulder, signs of infection like fever or warmth and redness around the joint, or symptoms suggesting something more serious like chest pain or difficulty breathing that might be mistaken for shoulder pain.
It’s also worth seeking professional guidance if you’ve been managing shoulder symptoms on your own for several weeks without improvement. Conservative care tends to be most effective when started early in the process, particularly during the transition from freezing to frozen stage.
| Frozen Shoulder Characteristics | Other Shoulder Conditions |
|---|---|
| Both active and passive motion severely restricted | Active motion may be limited, but passive motion often preserved |
| Gradual onset without specific injury | Often related to specific trauma or overuse event |
| Progressive worsening over months | Symptoms may fluctuate or improve with rest |
| Severe night pain in early stages | Night pain less characteristic |
| Follows predictable stage progression | May not follow specific pattern |
| External rotation most severely limited | Limitation pattern varies by condition |
Myths vs. Facts About Frozen Shoulder
Myth: Frozen shoulder only happens after an injury
Fact: While frozen shoulder can develop after trauma or surgery, it frequently occurs without any precipitating injury. Many patients develop frozen shoulder spontaneously, particularly those with diabetes or other risk factors. The “primary” or “idiopathic” form of frozen shoulder has no clear trigger, which is actually more common than the post-traumatic variety.
Myth: You should rest your shoulder completely and avoid movement
Fact: Complete immobilization will actually worsen frozen shoulder by allowing more adhesions to form and the capsule to tighten further. Gentle, consistent movement within comfortable ranges is crucial throughout all stages of recovery. The key is finding the balance between avoiding painful forced movements while maintaining mobility through regular, controlled motion.
Myth: Frozen shoulder resolves quickly with the right treatment
Fact: Frozen shoulder is a lengthy condition that typically takes 1-3 years to fully resolve, even with appropriate treatment. Conservative care can help manage pain, prevent further loss of function, and support the natural healing process, but there’s no quick fix. Setting realistic expectations is important for maintaining motivation throughout the recovery journey.
Myth: If one shoulder freezes, the other will too
Fact: While having frozen shoulder in one shoulder does somewhat increase the risk for the opposite shoulder, it doesn’t mean it will definitely happen. Studies suggest that about 5-15% of people who experience frozen shoulder in one shoulder will later develop it in the other, often within five years. This risk is higher than the general population but still means most people won’t experience bilateral frozen shoulder.
Myth: Surgery is the only effective treatment for frozen shoulder
Fact: The vast majority of frozen shoulder cases resolve with conservative care including chiropractic treatment, physical therapy, and self-management strategies. Guidelines from organizations like the American Academy of Orthopaedic Surgeons recommend trying conservative approaches for at least several months before considering more invasive interventions. Surgery is typically reserved for the small percentage of cases that don’t respond adequately to conservative management after an extended period.
Final Thoughts
Frozen shoulder can be one of the more challenging conditions to live with due to its prolonged nature and impact on daily function. However, understanding what you’re dealing with, recognizing which stage you’re in, and engaging in appropriate conservative care can make a significant difference in your comfort and recovery trajectory. While the journey to full recovery takes patience, most people do regain substantial function over time.
Here in Charlotte, the team at Chiropractic Fitness is experienced in helping patients navigate the complexities of frozen shoulder recovery. We understand the frustration of dealing with persistent pain and limitation, and we’re committed to providing individualized, evidence-based care that supports your body’s natural healing while helping you maintain the best possible function throughout the recovery process.
If you’re experiencing shoulder pain and stiffness that’s affecting your quality of life, don’t wait for symptoms to become severe before seeking help. Early evaluation and management can help you better understand your condition, learn effective strategies for managing symptoms, and begin working toward recovery. Whether you’re in the painful freezing stage or working through the gradual improvements of the thawing stage, professional guidance can help you navigate each phase more effectively and with greater confidence in your recovery.
Frequently Asked Questions
How long does frozen shoulder typically last?
Frozen shoulder generally lasts between 1-3 years from onset to full recovery, though the timeline varies significantly between individuals. The freezing stage lasts 2-9 months, the frozen stage 4-12 months, and the thawing stage 6 months to 2 years. Some people experience faster recovery while others take longer, but most see substantial improvement over time with or without treatment.
Can I still exercise with frozen shoulder?
Yes, maintaining appropriate exercise is actually important for frozen shoulder recovery. Focus on gentle range-of-motion exercises, pendulum movements, and activities that don’t aggravate your pain. Avoid high-impact activities that stress the shoulder or movements that cause sharp pain. Your chiropractor can provide specific exercises appropriate for your current stage and tolerance level.
Why does frozen shoulder hurt more at night?
Night pain is common with frozen shoulder for several reasons. When you’re lying down, there’s less gravitational distraction on the joint, which can increase compression and discomfort. Inflammatory chemicals tend to accumulate during inactivity, and you may unconsciously move the shoulder into positions that stress the tight capsule while sleeping. Additionally, distraction from daytime activities is absent, making pain more noticeable.
Will my frozen shoulder come back after it heals?
Recurrence of frozen shoulder in the same shoulder is uncommon once it has fully resolved. However, there is a somewhat increased risk of developing frozen shoulder in the opposite shoulder, occurring in roughly 5-15% of cases, often within several years. Maintaining shoulder mobility and managing underlying risk factors like diabetes can help reduce these risks.
Is frozen shoulder the same as a rotator cuff tear?
No, these are distinct conditions though they can cause similar symptoms. Frozen shoulder involves capsular thickening and adhesions with equally restricted active and passive motion. Rotator cuff tears involve damaged tendons and typically show more restriction in active motion while passive motion may be relatively preserved. A thorough examination by a qualified practitioner can differentiate between these conditions.
Can diabetes really increase my risk of frozen shoulder?
Yes, diabetes is one of the strongest risk factors for developing frozen shoulder. People with diabetes have a 10-20% lifetime risk compared to 2-5% in the general population. The elevated blood sugar associated with diabetes may affect collagen in connective tissues, making the shoulder capsule more prone to inflammation and adhesion formation. Better blood sugar control may help reduce this risk.
TL;DR – Key Takeaways
- Frozen shoulder is a condition where the shoulder capsule thickens and tightens, causing progressive pain and severe motion restriction that typically resolves over 1-3 years through distinct freezing, frozen, and thawing stages
- Common risk factors include diabetes, thyroid disorders, prolonged shoulder immobility, age 40-60, and being female, though frozen shoulder often occurs without clear cause or preceding injury
- Chiropractic care offers conservative, non-surgical management focusing on pain reduction, maintaining mobility, and gradually restoring range of motion through manual therapy, mobilization, and therapeutic exercise
- Continuing gentle movement within comfortable ranges is crucial throughout recovery—complete immobilization worsens the condition by allowing more adhesions to form and further capsular tightening
- While recovery is lengthy, most people regain substantial shoulder function over time with appropriate conservative care, patience, and consistent engagement in therapeutic strategies tailored to each stage of the condition